- Conditions
- Ankle instability
Ankle instability Functional ankle instability / chronic ankle instability / frequent ankle sprains
Introduction
Ankle instability involves pain and a feeling of instability in the ankle. The symptoms usually occur as a result of previous ankle sprains. Ankle instability increases the risk of frequently spraining the ankle.
Ankle instability occurs in every age group. It is more commonly seen in athletes who play contact sports such as football.
Description of the condition
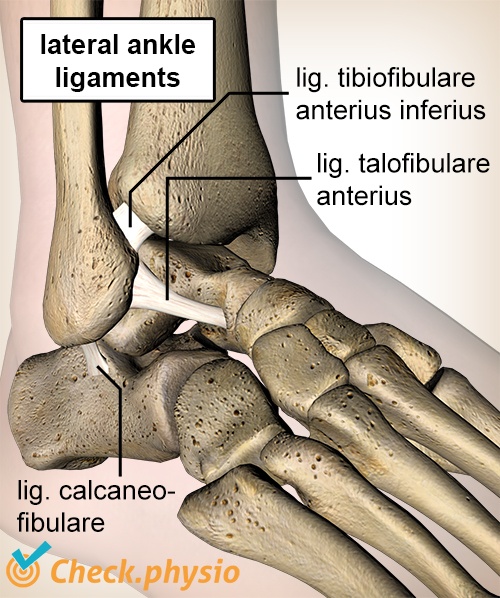
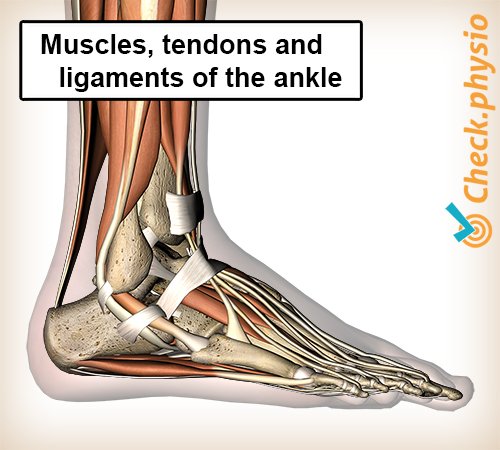
The ankle joint is firmly held together by the ankle ligaments and the muscles that move the ankle. Thanks to the interdependent muscular function and the strength provided by the ankle ligaments, the ankle feels 'stable'. Unfortunately, this can change if the ankle is damaged.
In an acute ankle sprain, the ankle usually tilts inwards, causing damage to the lateral ankle ligaments. Tearing the ankle ligaments causes the ends of the ankle ligaments to be further apart. As a result, ankle ligament injuries cause an immediate loss of stability (strength) in the ankle. This is referred to as ankle instability.
We differentiate between short-term and long-term ankle instability. Most of the time, ankle instability is short-term. The body recovers by itself again for instance after spraining your ankle. If the complaints last longer than 12 weeks, there is a structural loss of stability and this is referred to as long-term ankle instability.
Ankle instability that lasts longer than the normal recovery process is to be split into two categories. There is functional ankle instability and mechanical instability.
Functional ankle instability
In terms of functional instability, the ankle ligaments have recovered well, but the muscles are too weak or react insufficiently. This means that the body is unable to actively provide the right strength to the ankle.
The ankle ligaments, muscles and the joint capsule contain sensors that observe movement in the ankle. Since this is how your body gets information about movements in the joint, your muscles can react quickly if you are about to stumble. As a result of an ankle injury, these sensors can get damaged and not function as well. Consequently, it becomes a lot harder for your muscles to react quickly and correctly if you are about to sprain your ankle.
Mechanical ankle instability
In terms of mechanical ankle instability, the ankle ligaments are not strong enough or have not healed perfectly well. This is also referred to as laxity (weakness) of the ankle ligaments. As a result, there is too much mobility in the ankle joint so that the ankle remains unstable.
Combination
Ankle instability is often a combination of mechanical and functional instability. The ankle ligaments did not recover well or have become too long due to mechanical instability. The sensors in the ankle ligaments cannot function properly as a result thereof. If this is not trained after an acute ankle sprain, functional instability develops.
Cause and origin
Ankle instability is usually caused by a previous ankle sprain. Ankle instability can also be the result of a congenital abnormality of the ankle structures which should provide stability. This is however not common. Long-term ankle instability develops in 20% to 40% of people with an ankle sprain. To prevent long-term ankle instability from developing, it is important that an ankle sprain is treated properly.
Signs & symptoms
Persistent pain or frequent sprains are the most common symptoms of ankle instability. The pain is usually on the lateral side of the ankle. In addition, there is often a feeling of uncertainty when walking on uneven ground and there is a fear of new sprains during (sports) activities.
Symptoms of ankle instability:
- Feeling of uncertainty in the ankle when walking and/or playing sports.
- Frequently spraining the ankle.
- Pain in the area around the ankle, usually on the lateral side of the foot.
- Feeling of instability in the ankle when walking on uneven ground.
- Fluid in the ankle after straining.
Symptoms of functional instability:
- Disturbed coordination of the ankle.
- Loss of ankle stability.
- Loss of muscular strength in the ankle.
- Movement anxiety (not really daring to be weight-bearing on the ankle).
- Reduced mobility in the other joints of the ankle and foot.
Symptoms of mechanical instability:
- Increased mobility of the ankle as a result of ankle ligaments being too loose.
Diagnosis
An initial diagnosis is made on the basis of an interview with the physiotherapist. The latter will ask about previous ankle sprains and the feeling of instability at the time. This is followed by a physical examination to determine whether there is actual ankle instability.
For functional ankle instability, the degree of interdependent muscular function, coordination and muscle strength is assessed. Loss of coordination and stability can mainly be measured by tests on one leg. The affected ankle will have more difficulty stabilising and will tire more easily during these tests.
Mechanical instability can mainly be determined if there is laxity of the ankle ligaments. In addition, the mobility of each joint in the foot and the ankle is examined.
MRI can help make the right diagnosis. These additional examinations are initiated if another injury is suspected or to assess the quality of the ankle ligaments.
Treatment and recovery
The treatment of ankle instability depends on the results of the physical examination and the degree of activity of the patient. Non-surgical (conservative) treatment consists of physiotherapy, use of an ankle brace and/or medication. Medication is only used if an inflammation is present which does not disappear with rest.
Physiotherapy
Physiotherapy will always consist of exercise therapy aimed at coordination, balance, interdependent muscular function and muscle strength. If it is found that there is limited movement in the foot or ankle, a physiotherapist can treat this by ankle brace can be used to prevent new sprains. It is used primarily during sport activities. The use of an ankle brace is functional and does not result in a loss of stability of muscle strength in the long run. The ankle brace can be used in both mechanical and functional ankle instability. But a brace will be advised more if mechanical ankle instability is the cause.
Surgery
In some cases of mechanical ankle instability, surgery will be considered. The orthopaedic surgeon decides in consultation with the patient if surgery is desirable. The degree of instability, improperly reacting to previous treatments and the level of activity of the patient play an important role in this.
In terms of the level of activity, the occupation and/or level of sport of the patient are the most important pillars. Patients who sit down for their occupation will undergo surgery a lot less quickly than for instance soldiers. The same applies for top athletes require more use of their ankle than people who play sports at a lower level.
In case of surgery, the (lateral) ankle ligaments are repaired. The rehabilitation period usually lasts between 5 and 9 months before resuming sports. Due to this long rehabilitation period, patients often opt using a brace instead of surgery to prevent new sprains.
Exercises
To improve ankle stability, exercises are recommended. Follow the exercise programme with ankle instability exercises here.
More info
You can check your symptoms using the online physiotherapy check or make an appointment with a physiotherapy practice in your area.
References
Wees, Ph.J. van der, Lenssen, A.F., Feijts, Y.A.E.J., Bloo, H., Moorsel, S.R. van, Ouderland, R., Opraus, K.W.F., Rondhuis, G., Simons, A., Swinkels, R.A.H.M., Vaes, P., Verhagen, E., Hendriks, H.J.M., Bie, R.A. de (2006) KNGF-richtlijn. Enkelletsel Jaargang 116. Nummer 5. Update klinimetrie 2017.
Hiller, C.E., Kilbreath, S.L. & Refshauge, K.M. (2011) Chronic Ankle Instability. Evolution of the Model Faculty of Health Sciences, University of Sydney, New South Wales, Australia.
Fraser, J.J., Feger, M.A. & Hertel, J. (2016) Clinical commentary on midfoot and Forefoot involvement in lateral ankle sprains And chronic ankle instability. Part 2: clinical considerations The International Journal of Sports Physical Therapy. Volume 11, Number 7, December 2016.