- Conditions
- Tarsal coalition
Tarsal coalition Growth of the tarsal bones / talocalcaneal coalition
Introduction
Tarsal coalition is diagnosed when two tarsal bones have (partially) fused into one larger piece of bone. A tarsal coalition can be congenital or develop over time. A tarsal coalition does not always have to lead to problems. When symptoms do occur, pain and stiffness in the midfoot are the most prominent.
Tarsal coalition disorder occurs in about 1-2% of the people. In the congenital variant, complaints usually develop during puberty. Complaints that develop later in life are more likely the result of rheumatoid arthritis or develop after a traumatic joint injury.
Description of the condition
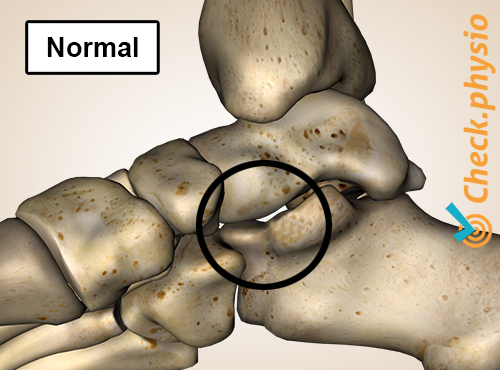
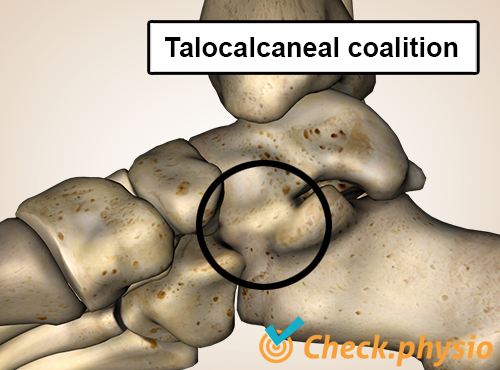
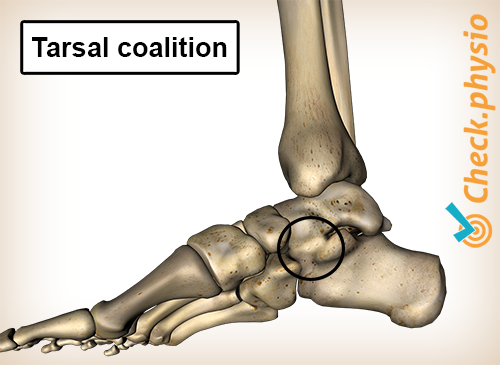
Normally, the tarsal bones consist of seven separate bones. In some people, two of these bones can fuse together to form a 'coalition'. The resulting joint connection can be made of bone, cartilage or connective tissue. In the case of bone tissue, the connection will be very stiff. In the case of connective tissue, the connection is still reasonably mobile. The stiffer the connection, the more likely it is to lead to complaints. Problems often arise elsewhere in the foot as well, because other joints are subjected to greater strain.
Tarsal coalitions are most frequently seen between the foot bones referred to as talus and calcaneus, and between calcaneus and the navicular bone. A connection may also develop between other tarsal bones.
Cause and origin
A tarsal coalition can be congenital but can also be the result of a joint disorder or an accident. When it’s a congenital disorder, it will appear in both feet in about 50% of the cases. The joint between the tarsal bones is already incorrectly formed at birth and develops into a tarsal coalition.
The moment at which the bones actually fuse, depends on the bones involved. Not all bones fuse together equally fast. Most congenital tarsal coalitions are mostly completed in the middle of puberty.
Complaints primarily develop before the age of 20. That is when the bones have fused and the strain on the joints often becomes greater because of sports. For example, even when someone sprains the ankle and does not recover well, this may be because of the presence of a tarsal coalition.
As for a non-congenital tarsal coalition, this is a disorder that has seriously affected the joint. Think of rheumatism, a fracture or infection. In a situation like that, the tarsal coalition can develop at any age.
Signs & symptoms
Possible complaints of tarsal coalition are:
- Pain in the midfoot.
- Stiffness of the midfoot (stiff foot or feet).
- A flatfoot that cannot be corrected.
- Frequently spraining the ankle.
- Increased complaints during or after activity.
Diagnosis
The correct diagnosis is sometimes missed if only an interview and physical examination are carried out. The physical examination can, however, reveal stiffness in certain joints. A flat foot may also be observed that cannot be corrected.
If the bones are completely fused together, the tarsal coalition can usually be seen clearly on an MRI can identify the problem in the first place when the connection between the bones does not (yet) consist of bone tissue.
Treatment and recovery
In order to reduce the symptoms resulting from a tarsal coalition, non-operative remedies are used first. Taking sufficient rest, fitting orthotics, taking painkillers and physiotherapy can help.
If the above is insufficiently effective, surgery can be performed. During surgery, the two bones are disconnected again. The aim of this is to improve the mobility of the foot and to reduce the pain.
When a joint is seriously affected, or has fused over a large area, the joint is often completely immobilised. This option can also be chosen if previous surgery has not helped. The disadvantage, however, is that the mobility of the foot will always be limited after this procedure. The activity pattern will have to be adjusted accordingly.
More info
You can check your symptoms using the online physiotherapy check or make an appointment with a physiotherapy practice in your area.
References
Wiendels, D.R., Aarts, N.J.M., Steenmeijer, V.A. & Smeets, H.J. (2009) Herkenning van een tarsale coalitie. Klinische en radiologische aanknopingspunten Ned Tijdschr Geneeskd. 2009;153:A616.
Nugteren, K. van & Winkel, D. (2009) Onderzoek en behandeling van de voet Houten: Bohn Stafleu van Loghum.
Verhaar, J.A.N. & Linden, A.J. van der (2005) Orthopedie Houten: Bohn Stafleu van Loghum.
Brukner, P. & Khan, K. (2010) Clinical sports medicine McGraw-Hill: Australia. 3e druk.