- Conditions
- Base of thumb arthritis
Base of thumb arthritis CMC-1 osteoarthritis / basal thumb wear and tear
Introduction
Base of thumb arthritis involves a problem with the joint of the thumb adjacent to the wrist. The joint is covered with a thin layer of cartilage. Base of thumb arthritis reduces the quality and density of the cartilage. As a result, daily activities can be more difficult and painful to perform.
In the past, base of thumb arthritis was more common with housewives. This was due to the fact that the disorder was more common in women who did a lot of household chores requiring a lot of squeezing and wringing. This does not mean that other people cannot suffer from base of thumb arthritis.
Description of the condition
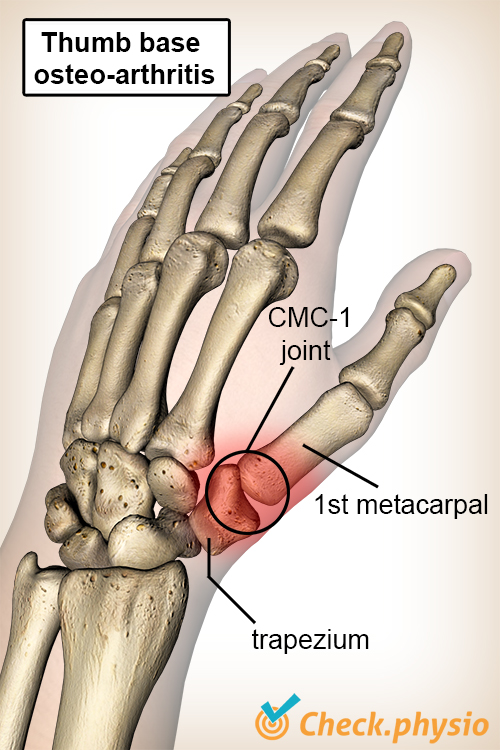
Base of thumb arthritis involves the joint referred to as the CMC-1 joint. This joint is located between one of the carpal bones (the os trapezium) and the first metacarpal bone (the os metacarpale I). It is also called a saddle joint because of its unique shape that makes the thumb much more mobile than the other fingers.
The tips of the bone in the joint are covered with a smooth layer osteoarthritis of the hand is seen more often in women. The risk of developing base of thumb arthritis increases as a person ages.
Cause and origin
The fact that the thumb is subjected to frequent and relatively heavy strain on a daily basis makes it susceptible to base of thumb arthritis. The joint is also more unstable due to the high degree of mobility. For stability, the joint depends on the rheumatoid arthritis.
Signs & symptoms
Complaints that occur in people with base of thumb arthritis are:
- (nagging) pain at the base of the thumb.
- Local swelling. - Loss of strength.
- Restriction of movement and stiffness.
- Cracking or grinding noises (crepitations).
- Difficulty squeezing, writing, wringing, opening jars, turning keys, etc.
- In more serious cases, the joint may deform and the thumb may become crooked.
Diagnosis
A doctor or (hand) physiotherapist will ask about the origin and consequences of the symptoms. This will be followed by a physical examination to look at the appearance and mobility of the thumb.
The grind test is a special test for the basal thumb joint which assesses pain and crepitations. In addition, several functional tests may be carried out to assess thumb strength and functionality. A possible x-ray confirms the diagnosis of base of thumb arthritis and also shows the severity of the osteoarthritis.
Treatment and recovery
In case of base of thumb arthritis, the initial advice is to put less strain on the thumb. This can be supported with medication and exercises. The latter is often done under the supervision of a (hand) physiotherapist.
In order to properly relieve the thumb joint, a splint may be used. This stabilises the joint when exerting pressure with the thumb. If this does not lead to sufficient improvement either, a referral to a hand surgeon may be appropriate. The surgeon may propose an injection or surgery.
Surgery
Surgery in case of base of thumb arthritis can be performed in different ways. For example, by removing the os trapezium or securing the basal joint of the thumb. To decide which method to use will depend on personal circumstances, the severity of the osteoarthritis and the extent to which the thumb will be used again after surgery.
Exercises
Take a look at the exercise programme with exercises for thumb base osteoarthritis.
More info
You can check your symptoms using the online physiotherapy check or make an appointment with a physiotherapy practice in your area.
References
Greving, J., Kok-Pigge, A., Kuijpers, T., Krastman, P., Peters-Veluthamaningal, C., de Vries, A., Wolters, R. (2021) NHG-Standaard. Hand- en polsklachten Nederlands Huisartsen Genootschap. Versie 3.0, februari 2021.
