- Conditions
- Leg thrombosis
Leg thrombosis Deep vein thrombosis / DVT
Introduction
A leg with thrombosis is a condition where a blood clot forms in the blood vessels of the lower leg. Such a blood clot can cause a blood vessel to close off completely or partially.
Description of the condition
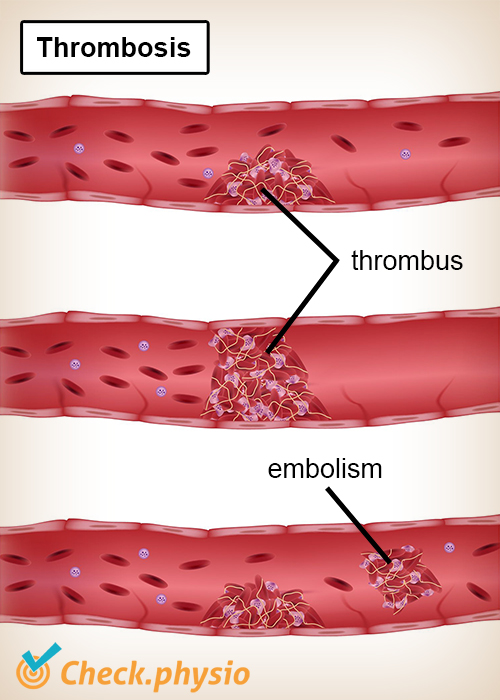
A leg with thrombosis involves a blood clot inside a blood vessel. We call this blood clot a thrombus. A thrombus is attached to the blood vessel wall at the place where it formed. This can be in a vein or an artery.
Blood clotting is normally very important to prevent blood loss during injuries. Blood clotting is what turns the liquid blood, which flows out of a blood vessel during an injury, into a jelly-like mass that stops the bleeding.
In legs with thrombosis, a blood clot in a vein of the leg causes problems. The blood clot obstructs the blood flow. This causes the leg to swell and feel heavy. Arteries have a much higher blood flow than veins. Therefore, blood clotting in the arteries is less frequent.
Embolism
When a piece or whole blood clot detaches from the blood vessel wall it is carried away by the blood flow. If this clot then gets stuck in another vein or artery, we call this an embolism. The best known form of an embolism is a pulmonary embolism.
Other forms of thrombosis
The best known form of thrombosis is leg thrombosis. There are also other lesser-known forms of thrombosis. In eye thrombosis there is a blood clot in the blood vessels of the retina and in sinus thrombosis there is a blood clot in the draining blood vessels of the head. Thrombosis can also occur in the arm, which is called a arm thrombosis.
Cause and origin
Thrombosis can be caused, among other things, by an irregular blood flow or by blood vessels that are no longer smooth inside (arteriosclerosis). An altered composition of the blood can also cause thrombosis.
The greatest risk factor for developing thrombosis is previously experienced thrombosis. There are also a number of other risk factors that increase the risk of thrombosis. However, thrombosis can also occur without the presence of obvious risk factors.
Thrombosis can occur when the quality of the blood vessels is impaired by:
- Smoking.
- High cholesterol levels.
- Diabetes.
- High blood pressure.
- Cancer.
In addition, thrombosis can also occur when blood flow becomes too slow. This prevents the blood from flowing properly, after which thrombosis can occur. Slowed blood flow can be caused by prolonged bed rest, surgery, plaster casts, long plane or bus journeys and cardiac arrhythmia, among other things.
The composition of the blood can also affect thrombosis. When the blood is too thick, the flow is impeded. This is caused, for example, by an excess of blood cells or by a shortage of inhibitors that must inhibit blood coagulation.
Thrombosis is more common in certain families than in others. This is usually because these families are genetically predisposed to cardiovascular diseases.
Signs & symptoms
Thrombosis can manifest itself in various ways. This depends on the location of the thrombosis. However, there are a number of important features that can indicate thrombosis in a leg:
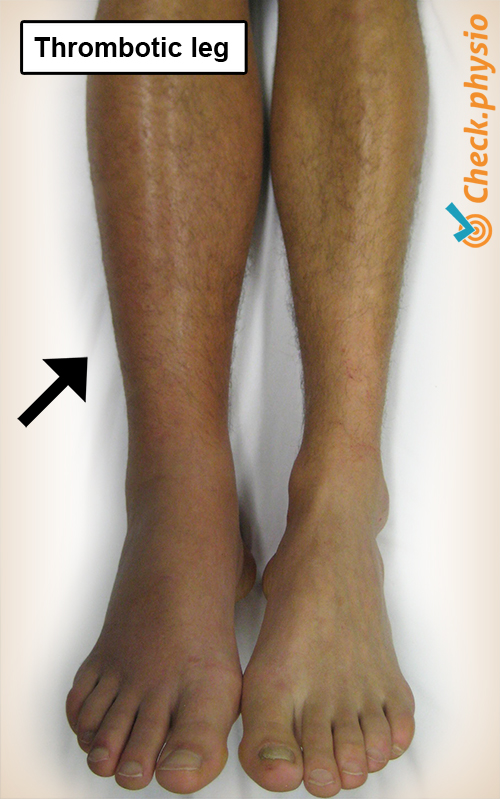
- Fairly rapid swelling in one leg.
- Feeling of heaviness in one leg.
- A red or bluish discolouration in one leg.
- Possibly an increase in temperature.
- Tight skin, possibly red and shiny.
The swelling and the swollen feeling in the leg are caused by the fact that the blood vessels can no longer drain the blood and the fluids carried along properly. The lymphatic vessels play an important role in the drainage of fluid. As a result of the thrombosis, the lymphatic vessels cannot function as well, making it more difficult for them to drain the fluid.
The discolouration in the leg is caused by the increased pressure in the blood vessels. A similar phenomenon is seen when blood is drawn. A band is put around the arm to increase the pressure. This pushes the vein to the surface, making it more visible. This can also occur with thrombosis and explains the discolouration in the leg.
The above symptoms do not always all have to be present. In addition, the symptoms can also indicate other conditions. One in four people with the above symptoms actually has leg thrombosis. The advice is; always consult a doctor in case of suspicion.
Diagnosis
The diagnosis is made by a doctor. A blood test will also be carried out to check the blood's ability to coagulate.
Treatment and recovery
Leg thrombosis is easy to treat. However, if left untreated, a pulmonary embolism may occur. Therefore, in case of suspicion, it is always important to consult a doctor.
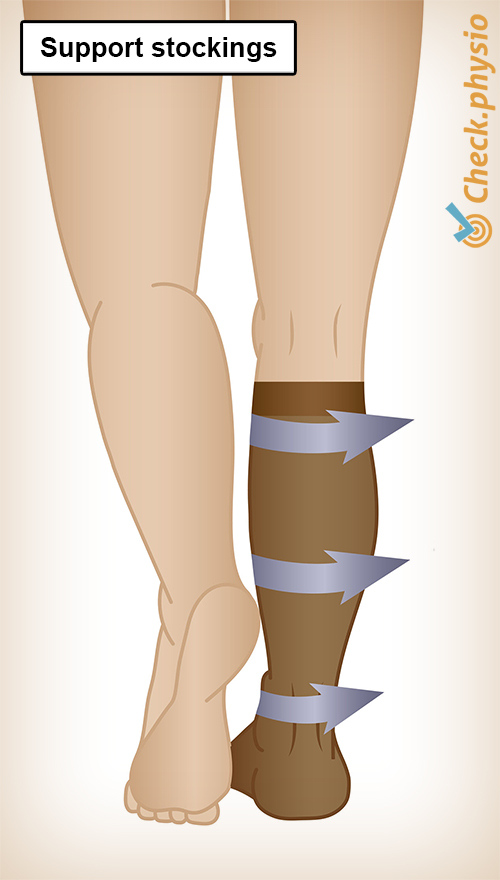
Thrombosis will always be treated with drugs. In addition, elastic stockings are often used in the treatment of thrombosis. These stockings improve blood circulation and ensure that excess fluid in the leg is drained off.
After thrombosis, preventing subsequent thrombosis is very important. One way of doing this is to continue to use medication and elastic stockings. In addition, a healthy lifestyle is very important:
- Sufficient physical activity.
- Avoid long periods of sitting.
- A healthy diet, to keep cholesterol down.
- Quitting smoking, if possible.
More info
You can check your symptoms using the online physiotherapy check or make an appointment with a physiotherapy practice in your area.
References
Prenatali, E., Bucciarelli, P., Passamonti, S.M. & Martinelli, I. (2011) Risk factors for venous and arterial thrombosis A. Bianchi Bonomi Haemophilia and Thrombosis Centre, IRCSS General Hospital, Mangiagalli and Regina Elena Foundation, Milan, Italy.
Nugteren, K. van & Winkel, D. (2008) Onderzoek en behandeling van spieraandoeningen en kuitpijn Houten: Bohn Stafleu van Loghum.
Oudega, R., Van Weert, H., Stoffers, H.E.J.H., Sival, P.P.E., Schure, R.I., Delemarre, J., Eizenga, W.H. (2015) NHG-Standaard. Diepe veneuze trombose en longembolie Huisarts Wet 2008;51(1):24-37.